What Is the Last Bone to Complete Its Growth
Learning Outcomes
- Depict how bones develop, abound, and repair
Ossification, or osteogenesis, is the process of bone germination by osteoblasts. Ossification is distinct from the process of calcification; whereas calcification takes place during the ossification of bones, it can also occur in other tissues. Ossification begins approximately vi weeks afterwards fertilization in an embryo. Before this fourth dimension, the embryonic skeleton consists entirely of fibrous membranes and hyaline cartilage. The development of os from fibrous membranes is called intramembranous ossification; evolution from hyaline cartilage is chosen endochondral ossification. Bone growth continues until approximately age 25. Bones can grow in thickness throughout life, but subsequently age 25, ossification functions primarily in os remodeling and repair.
Intramembranous Ossification
Intramembranous ossification is the procedure of bone development from fibrous membranes. It is involved in the formation of the flat bones of the skull, the mandible, and the clavicles. Ossification begins equally mesenchymal cells form a template of the time to come os. They and then differentiate into osteoblasts at the ossification center. Osteoblasts secrete the extracellular matrix and deposit calcium, which hardens the matrix. The non-mineralized portion of the bone or osteoid continues to form around blood vessels, forming spongy bone. Connective tissue in the matrix differentiates into red bone marrow in the fetus. The spongy bone is remodeled into a thin layer of compact bone on the surface of the spongy bone.
Endochondral Ossification
Endochondral ossification is the process of bone evolution from hyaline cartilage. All of the bones of the torso, except for the flat bones of the skull, mandible, and clavicles, are formed through endochondral ossification.
In long basic, chondrocytes class a template of the hyaline cartilage diaphysis. Responding to circuitous developmental signals, the matrix begins to lapidify. This calcification prevents diffusion of nutrients into the matrix, resulting in chondrocytes dying and the opening up of cavities in the diaphysis cartilage. Blood vessels invade the cavities, and osteoblasts and osteoclasts modify the calcified cartilage matrix into spongy bone. Osteoclasts then break down some of the spongy os to create a marrow, or medullary, cavity in the center of the diaphysis. Dense, irregular connective tissue forms a sheath (periosteum) around the bones. The periosteum assists in attaching the bone to surrounding tissues, tendons, and ligaments. The bone continues to grow and elongate as the cartilage cells at the epiphyses dissever.
In the last stage of prenatal os development, the centers of the epiphyses begin to calcify. Secondary ossification centers class in the epiphyses every bit blood vessels and osteoblasts enter these areas and catechumen hyaline cartilage into spongy bone. Until boyhood, hyaline cartilage persists at the epiphyseal plate (growth plate), which is the region between the diaphysis and epiphysis that is responsible for the lengthwise growth of long basic (Figure 1).
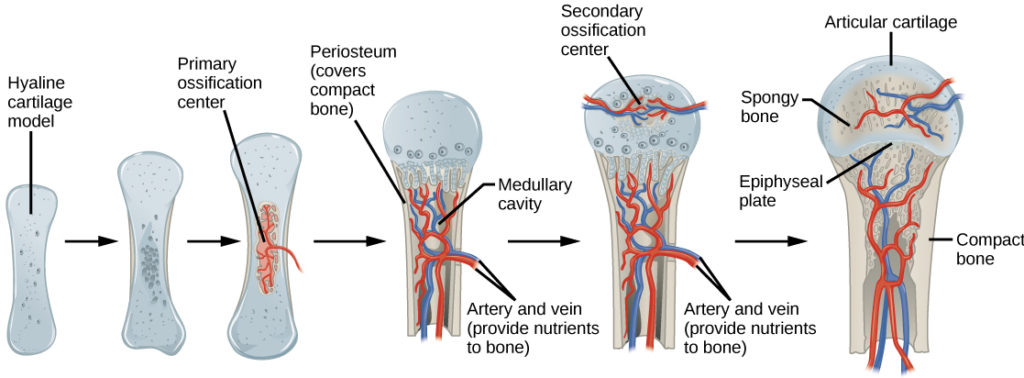
Figure 1. Endochondral ossification is the process of bone development from hyaline cartilage. The periosteum is the connective tissue on the outside of os that acts as the interface betwixt bone, blood vessels, tendons, and ligaments.
Growth of Os
Long basic go on to lengthen, potentially until adolescence, through the addition of bone tissue at the epiphyseal plate. They also increase in width through appositional growth.
Lengthening of Long Bones
Chondrocytes on the epiphyseal side of the epiphyseal plate carve up; ane cell remains undifferentiated virtually the epiphysis, and i jail cell moves toward the diaphysis. The cells, which are pushed from the epiphysis, mature and are destroyed by calcification. This process replaces cartilage with bone on the diaphyseal side of the plate, resulting in a lengthening of the os.
Long basic stop growing at around the age of eighteen in females and the age of 21 in males in a process chosen epiphyseal plate closure. During this process, cartilage cells stop dividing and all of the cartilage is replaced by bone. The epiphyseal plate fades, leaving a structure called the epiphyseal line or epiphyseal remnant, and the epiphysis and diaphysis fuse.
Thickening of Long Basic
Appositional growth is the increment in the diameter of bones by the improver of bony tissue at the surface of bones. Osteoblasts at the os surface secrete bone matrix, and osteoclasts on the inner surface break downward bone. The osteoblasts differentiate into osteocytes. A balance between these two processes allows the bone to thicken without becoming too heavy.
Bone Remodeling and Repair
Bone renewal continues after birth into adulthood. Bone remodeling is the replacement of sometime os tissue by new bone tissue. It involves the processes of os deposition by osteoblasts and bone resorption by osteoclasts. Normal bone growth requires vitamins D, C, and A, plus minerals such every bit calcium, phosphorous, and magnesium. Hormones such as parathyroid hormone, growth hormone, and calcitonin are also required for proper bone growth and maintenance.
Bone turnover rates are quite high, with 5 to seven pct of bone mass being recycled every week. Differences in turnover rate exist in different areas of the skeleton and in different areas of a bone. For case, the bone in the head of the femur may be fully replaced every 6 months, whereas the bone forth the shaft is contradistinct much more than slowly.

Effigy 2. Later on this bone is ready, a callus will knit the two ends together. (credit: Nib Rhodes)
Os remodeling allows basic to adapt to stresses by becoming thicker and stronger when subjected to stress. Bones that are not subject to normal stress, for case when a limb is in a cast, volition begin to lose mass. A fractured or broken bone undergoes repair through iv stages:
- Blood vessels in the cleaved bone tear and hemorrhage, resulting in the germination of clotted claret, or a hematoma, at the site of the intermission. The severed blood vessels at the cleaved ends of the os are sealed by the clotting process, and bone cells that are deprived of nutrients begin to die.
- Within days of the fracture, capillaries grow into the hematoma, and phagocytic cells begin to clear away the dead cells. Though fragments of the blood jell may remain, fibroblasts and osteoblasts enter the surface area and brainstorm to reform bone. Fibroblasts produce collagen fibers that connect the broken bone ends, and osteoblasts start to form spongy os. The repair tissue betwixt the cleaved os ends is called the fibrocartilaginous callus, as information technology is equanimous of both hyaline and fibrocartilage (Figure two). Some bone spicules may also appear at this betoken.
- The fibrocartilaginous callus is converted into a bony callus of spongy os. It takes virtually 2 months for the broken bone ends to be firmly joined together later the fracture. This is similar to the endochondral formation of bone, as cartilage becomes ossified; osteoblasts, osteoclasts, and os matrix are nowadays.
- The bony callus is then remodelled by osteoclasts and osteoblasts, with backlog textile on the outside of the bone and within the medullary crenel being removed. Compact bone is added to create bone tissue that is like to the original, unbroken bone. This remodeling tin take many months, and the bone may remain uneven for years.
Decalcification of Bones
Question: What effect does the removal of calcium and collagen take on bone construction?
Background: Deport a literature search on the role of calcium and collagen in maintaining bone structure. Conduct a literature search on diseases in which os construction is compromised.
Hypothesis: Develop a hypothesis that states predictions of the flexibility, force, and mass of bones that accept had the calcium and collagen components removed. Develop a hypothesis regarding the attempt to add calcium back to decalcified bones.
Test the hypothesis: Test the prediction by removing calcium from craven bones by placing them in a jar of vinegar for vii days. Test the hypothesis regarding adding calcium back to decalcified bone by placing the decalcified chicken basic into a jar of water with calcium supplements added. Examination the prediction by denaturing the collagen from the bones past baking them at 250°C for three hours.
Clarify the data: Create a table showing the changes in bone flexibility, force, and mass in the three unlike environments.
Written report the results: Under which conditions was the bone most flexible? Nether which weather condition was the bone the strongest?
Describe a conclusion: Did the results support or refute the hypothesis? How do the results observed in this experiment represent to diseases that destroy os tissue?
IN SUMMARY: Bone Growth and Evolution
Ossification is the procedure of os formation by osteoblasts. Intramembranous ossification is the process of os development from fibrous membranes. Endochondral ossification is the procedure of bone development from hyaline cartilage. Long bones lengthen as chondrocytes dissever and secrete hyaline cartilage. Osteoblasts replace cartilage with os. Appositional growth is the increase in the diameter of bones by the addition of bone tissue at the surface of bones. Bone remodeling involves the processes of os degradation by osteoblasts and os resorption by osteoclasts. Bone repair occurs in 4 stages and tin have several months.
Endeavor It
Contribute!
Did you lot have an idea for improving this content? We'd love your input.
Improve this pageLearn More
hernandezentes1943.blogspot.com
Source: https://courses.lumenlearning.com/wm-biology2/chapter/bone-growth-and-development/
0 Response to "What Is the Last Bone to Complete Its Growth"
Post a Comment